February is the month of love, so love your heart
Published 11:01 am Monday, February 12, 2024
After President Lyndon B. Johnson had a heart attack in 1964, he issued the first proclamation proclaiming February American Heart Month. Every president since has followed his lead, and with good cause, since every 33 seconds one person dies from cardiovascular disease, making it the number one killer of Americans.
While strides have been made to combat heart disease, in an article published by the Center for Disease Control, it stated it has continued to remain the number one killer because people are unaware that it tops the list as the most life-threatening illness.
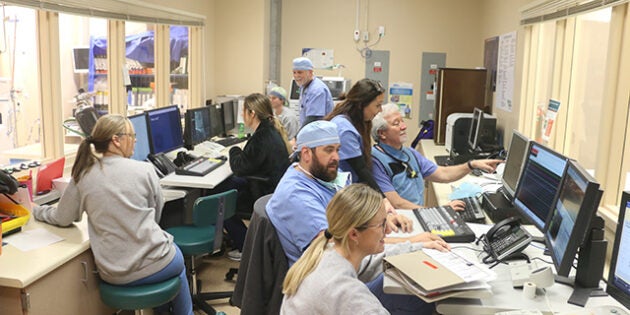
With that in mind, The Vicksburg Post sat down with Merit Health River Region’s interventional cardiologist Dr. Paul Pierce IV to talk about heart disease with hopes the information will educate people and ultimately aid in saving lives.
What is a heart attack?
Pierce: There are a couple of reasons that people can have heart attacks, but the primary cause is when a cholesterol-containing deposit builds up over time, forming a plaque inside the wall of the artery to the heart. The plaque can rupture, leading to the contents of the plaque spilling out into the bloodstream, which causes a blood clot. This blood clot can severely reduce or completely block the blood flow to the heart muscle, which leads to heart muscle damage, which is a heart attack.
Are there any early warning signs, or does a heart attack just happen all of the sudden?
Pierce: There can be early warning signs. Any sort of chest pressure that is brought on with exertion and relieved with rest can be a red flag. The symptoms are oftentimes associated with nausea, possible vomiting, diaphoresis (breaking out in a sweat), shortness of breath. Those can all be signs that the heart muscle is not getting the blood flow that it needs. This is called angina. But, often, a heart attack is a sudden thing. There is a plaque in the artery that does not restrict blood flow that, for reasons that are poorly understood, suddenly ruptures causing a blood clot. When that happens, the symptom complex occurs suddenly. And frequently the symptoms mentioned above all occur suddenly at once — chest pain/nausea/vomiting/breaking out in a sweat/shortness of breath. This is a medical emergency.
What does a person feel when they are actively experiencing a heart attack — male and female?
Pierce: The symptom complex can vary widely, not only between men and women, but person-to-person. Some people describe it as a pressure-like sensation, an “elephant on my chest” radiation of the pain into the jaw, into the shoulder, or through to the back. They may or may not break out in a sweat. There may or may not be nausea or vomiting. Some people have described it as an indigestion type sensation. Some people have pain in the epigastric area (upper abdomen). Basically, there are classic symptoms of a heart attack and less typical symptoms, but anything that is new/different/concerning needs to be evaluated/investigated.
Should a person having what seems like it could be a heart attack call 911 or should they have a family member or friend drive them to the hospital?
Pierce: If you are concerned (or think) that you are having a heart attack, you should immediately call 911. There are bad things that can happen that the ambulance crew will be prepared for, and that your family member who is driving you to the hospital will almost certainly not be prepared for.
What is the first thing that happens to a person when they are brought into the hospital? Are they rushed to surgery? Are tests done?
Pierce: If you are brought to the emergency room with concerns about having a heart attack, you will be immediately brought in for evaluation. There should not be any waiting around in the holding area/waiting room. An EKG is generally done within the first five minutes of presentation, and that can give us immediate indication whether the person is having a heart attack or not. After that, there will be lab work and further testing done, depending on the EKG and results of the blood tests.
There are certain types of heart attacks that are immediately rushed to the procedure room.
Are there different kinds of heart attacks and if so, are there different types of treatments and how are these procedures done?
Pierce: Yes, there are different types of heart attacks. The most concerning type of heart attack is what we call a “STEMI” or an ST elevation myocardial infarction. That is the heart attack that immediately gets rushed to the procedure room. The other type of heart attack is called a “NSTEMI” or a non-ST elevation myocardial infarction.
There are seven different types of heart attack.
Type 1: Caused by plaque rupture – this is the kind of heart attack that everyone thinks about when they think about a “heart attack.”
Type 2: This is a supply demand mismatch. This can occur when the heart rate is too high, or there is not enough blood to carry oxygen, or there is a lack of oxygen to the heart muscle.
Type 3: Sudden cardiac death (“dropped dead”) with symptoms of a heart attack or heart attack detected at autopsy
Type 4A: Procedure-related heart attack less than 48 hours after stent/balloon
Type 4B: Heart attack due to sudden stent blockage
Type 4C: Heart attack related to stent narrowing
Type 5: Heart attack/myocardial injury following coronary artery bypass surgery
The type of treatment is very patient-dependent. Each situation is unique in itself. Primarily, basic treatment is blood thinners/antiplatelet medications, and narcotics to help control pain, and medications to help the heart function return to normal. Procedurally speaking, patients often have an echocardiogram (an ultrasound test of the heart to let us look at the heart pump function and valves) and usually a coronary angiography/heart catheterization which helps us get a good look at the arteries and = which vessel is causing the problem. Most of the heart catheterizations these days are performed through an artery on the thumb side of the wrist, the radial artery. This is not surgery. There is no cutting, stitches, staples, or scalpel involved. It is a procedure, not a surgery. There is no breathing tube down the throat. We give the patients medication to help them relax, numb up the area, and proceed. Once we get past the numbing portion there is very little, if any, pain.
What is the recovery time after a heart attack?
Pierce: It depends on the size of the heart attack, which is usually determined by how high a lab value, called troponin, rises after the event. Troponin is a protein that is involved in heart muscle contraction and can follow that piece of lab work to tell us how big the heart attack is. Usual recovery time after a big heart attack is four to six weeks.
Can a person resume their normal life after a heart attack? and if not, what should they expect?
Pierce: Yes, a person can resume their normal life after a heart attack. There are many factors that can affect that. If there is a delayed presentation, and the artery is large and completely blocked, then you can have a significant area of heart muscle that is significantly damaged, leading to a permanent decrease in heart pump function. Patients that experience this have what we call “heart failure.” Those people require specialized medications and certain dietary restrictions.
What does heart disease mean? And what are the symptoms?
Pierce: Heart disease is an umbrella term that describes any type of disease process that affects the heart or related blood vessels. There are multiple risk factors for this, including high blood pressure/bad cholesterol/diabetes/smoking or secondhand smoke exposure/obesity/poor diet/sedentary lifestyle or physical inactivity. This can lead to high blood pressure, coronary artery disease or blockage in the heart arteries, peripheral vascular disease or blockage in the legs, carotid artery disease or blockage in the arteries to the brain, and stroke. The symptoms for these are various, as you can imagine.
Why do blood pressure and cholesterol levels matter when it comes to heart health?
Pierce: As they are part of the risk factor profile for evaluating someone who is at high risk for cardiovascular disease. As outlined above, these risk factors include high blood pressure, high cholesterol, diabetes, smoking or secondhand smoke exposure, poor diet, sedentary lifestyle. All of these can increase your risk for having a cardiac event. Anecdotally speaking, the two most potent contributing factors to coronary artery disease are poorly controlled diabetes and smoking. Diabetic smokers are at the highest risk.
Do some people have heart trouble even if they live a healthy lifestyle? And if so, why?
Pierce: Yes. Unfortunately, some patients have heart trouble even if they do everything right. Generally speaking, these patients have a genetic predisposition to coronary artery disease or have a “family history” of significant coronary artery disease. This is something that the patient really cannot do anything about other than try to prevent it with certain medications, and be aggressive with what we call primary prevention, which is preventing a cardiovascular event from happening in the first place. Oftentimes we are practicing what we call secondary prevention, which is after you have had an event like a heart attack or stroke we try to prevent another event from occurring.
What is a heart healthy lifestyle?
Pierce: There are many things people can do to lead a heart healthy lifestyle. These include maintaining a healthy weight, alcohol in moderation, not smoking or abusing tobacco products, exercise/be physically active, have a healthier diet, managing stress, getting enough sleep, and taking control of your own health care. We as physicians have responsibility in taking care of patients from a procedural standpoint, interpreting tests, and making sure patients are on the correct medications. However, the patient has a significant responsibility as well. This involves understanding their own risk for coronary artery disease, making healthy lifestyle choices, and taking appropriate steps to reduce chances of getting heart disease as outlined above. By taking these preventive measures, the patient can lower their risk of developing heart disease and improve their overall health and wellbeing.